Suffering extends beyond physical symptoms, encompassing emotional, social, and spiritual dimensions. Palliative care addresses this holistic need through a team-based approach, supporting patients and their families facing serious illnesses. This comprehensive care includes practical assistance, emotional support, and bereavement counseling, aiming to enhance the quality of life for patients until death by enabling them to live as actively as possible. Recognized as a human right, palliative care should be integral to person-centered health services, tailored to individual needs and preferences within a national health care program.
Defining Palliative Care and its Scope within a National Program
Palliative care is not limited to any specific disease but is crucial for a wide spectrum of conditions. While often associated with cancer, the reality is that the majority of adults requiring palliative care suffer from chronic illnesses such as cardiovascular diseases, chronic respiratory diseases, AIDS, and diabetes. Kidney failure, liver disease, neurological conditions like multiple sclerosis and Parkinson’s, dementia, and even drug-resistant tuberculosis are among the many other conditions where palliative care significantly improves patient well-being. A national health care program must recognize this broad applicability and ensure palliative care is accessible for all who need it, regardless of their diagnosis.
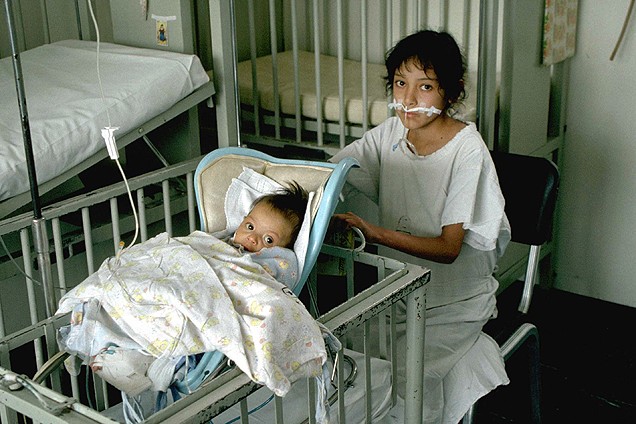 A health worker comforts a child receiving palliative care.
A health worker comforts a child receiving palliative care.
Alt text: A compassionate health worker provides comfort to a young child receiving palliative care, highlighting the human-centered approach.
Pain and breathlessness are prevalent and distressing symptoms for patients needing palliative care. A significant percentage of individuals with AIDS, cancer, cardiovascular disease, or chronic obstructive pulmonary disease experience moderate to severe pain as they near the end of life. Opioids are essential medications for managing this pain and alleviating breathlessness, underscoring the ethical imperative to control these symptoms early and respect patient dignity within a national health care framework.
Key Components of a National Health Care Program Integrating Palliative Care
A robust national health care program that effectively integrates palliative care requires several key components. These components ensure that palliative care is not a separate entity but a seamless and accessible part of the overall health system.
Policy and Integration
National health policies must explicitly include palliative care, integrating its services into the structure and financing of the national health care system at all levels. This integration should link palliative care with existing prevention, early detection, and treatment programs, creating a continuum of care that addresses needs from diagnosis to end-of-life.
Training and Human Resources
A critical element is strengthening and expanding human resources dedicated to palliative care. This includes comprehensive training for current health professionals and embedding palliative care education into the core curricula for all new health professionals. Furthermore, educating volunteers and the public is essential to build community support and understanding of palliative care.
Medicines and Accessibility
A national medicines policy must guarantee the availability of essential medicines for symptom management, particularly opioid analgesics for pain and respiratory distress. Addressing regulatory barriers and improving delivery systems are crucial to ensure that these medications are accessible to all patients in need, combating the global disparity in opioid consumption for palliative care.
Early Integration
Palliative care is most beneficial when introduced early in the course of a serious illness. Early palliative care not only enhances the patient’s quality of life but also demonstrably reduces unnecessary hospitalizations and the overall utilization of health care services, making it a cost-effective and patient-centered approach within a national program.
Universal Health Coverage and Equity
Palliative care must be provided in alignment with the principles of universal health coverage. Access should be guaranteed for all individuals, regardless of income, disease, or age. National programs need to incorporate financial and social protection mechanisms to ensure equitable access to palliative care, particularly for poor and marginalized populations, upholding the human right to health.
Multidisciplinary Teams
Palliative care delivery relies on multidisciplinary teams, and nurses are a vital part of this workforce. National programs should prioritize palliative care skills training for nurses, especially those working with seriously ill patients, empowering them to provide essential care and support.
Community and Home-Based Care
While specialist palliative care is a component, a sustainable and accessible system needs to be integrated into primary health care, community-based services, and home care settings. Supporting informal caregivers like family and community volunteers is also crucial. Providing palliative care should be recognized as an ethical responsibility for all health professionals within a national framework.
Overcoming Barriers to Palliative Care in National Programs
Despite its recognized importance, significant barriers hinder the widespread implementation of palliative care within national health programs. These barriers need to be actively addressed to improve access and ensure effective service delivery.
One major obstacle is the lack of integration of palliative care into national health policies and systems. Often, palliative care is overlooked or considered a niche service, rather than a fundamental component of comprehensive health care. Limited or nonexistent training for health professionals in palliative care further exacerbates the issue, leaving a workforce unprepared to meet patient needs. Inadequate access to opioid pain relief, often due to overly restrictive regulations or misconceptions, also prevents effective symptom management.
Beyond systemic issues, a lack of awareness among policymakers, health professionals, and the public about the nature and benefits of palliative care contributes to underutilization. Cultural and social beliefs surrounding death and dying can also create barriers, as can misconceptions that palliative care is only for cancer patients or those in the very final stages of life. Furthermore, unfounded fears that improved opioid access will lead to increased substance abuse can restrict necessary pain management.
WHO’s Role in Supporting National Palliative Care Programs
The World Health Organization (WHO) plays a crucial role in guiding and supporting member states in developing and strengthening national palliative care programs. Palliative care medicines are included in the WHO Essential Medicines List, signifying their importance in basic healthcare. WHO actively promotes the integration of palliative care into global health strategies related to universal health coverage and noncommunicable diseases.
WHO’s efforts include assessing the development of palliative care services worldwide, developing guidelines and tools for integrated palliative care across various diseases and care levels, and supporting member states in improving access to palliative care medicines through better regulations and delivery systems. The organization also focuses on specific areas like palliative care for people living with HIV and children, monitors global access, and encourages resource allocation for palliative care programs and research, particularly in resource-limited settings. WHO’s 2014 resolution urging member states to improve palliative care access as a core component of health systems highlights the global commitment to this essential aspect of healthcare.
Integrating palliative care into a national health care program is not merely an aspirational goal but a fundamental requirement for a humane and effective health system. By addressing policy, training, access to medicines, and overcoming societal barriers, nations can build health programs that truly prioritize patient well-being and dignity throughout the course of serious illness, ensuring that palliative care is available to all who need it.