Introduction to Longitudinal Care Programs
In today’s complex healthcare landscape, patients often navigate a fragmented system, transitioning between various care settings such as hospitals, emergency departments, skilled nursing facilities, and home healthcare agencies. This journey can be particularly challenging for individuals with chronic conditions or complex healthcare needs. Effective communication and coordinated care are paramount to ensuring patient safety, improving health outcomes, and enhancing the overall patient experience. A critical tool emerging to address these challenges is the Longitudinal Care Program (LCP). But what is a longitudinal care program exactly, and why is it becoming increasingly important?
This article delves into the concept of longitudinal care programs, exploring their definition, benefits, current state of implementation, and the strategies needed to realize their full potential. Drawing insights from a comprehensive study on care plan communication across different healthcare settings in the United States, we will illuminate the gaps in current practices and underscore the urgent need for widespread adoption of LCPs to transform healthcare delivery.
Understanding Longitudinal Care Plans: Definition and Core Principles
To truly understand what is a longitudinal care program, it’s essential to define its core components and principles. At its heart, a Longitudinal Care Plan (LCP) is a holistic, dynamic, and patient-centered blueprint that documents a patient’s health journey over time. It’s not merely a static document but a living, evolving plan that adapts to the patient’s changing needs and circumstances across different healthcare settings and levels of care.
Key characteristics of an LCP include:
- Holistic: An LCP considers the patient as a whole person, encompassing not just their medical conditions but also their social, emotional, and functional needs. It aims to integrate all aspects of care, from disease prevention to treatment and wellness goals.
- Dynamic: Unlike traditional care plans that are often setting-specific and fragmented, an LCP is designed to be continuously updated and refined as the patient’s health status evolves and as they move through different care environments. This dynamism ensures that the plan remains relevant and responsive to the patient’s current needs.
- Integrated: An LCP serves as a central repository of patient information, pulling together data from various sources, including electronic health records (EHRs), specialist reports, and patient-reported outcomes. This integration provides a comprehensive view of the patient’s health history and care plan, accessible to all authorized stakeholders.
- Patient-Centered: At its core, an LCP is designed to reflect the patient’s values, preferences, and goals. It emphasizes shared decision-making, ensuring that patients are active participants in shaping their care plan and are empowered to manage their health effectively.
- Actionable: An effective LCP provides actionable information to healthcare providers, patients, and their families. It outlines clear steps, interventions, and goals, facilitating proactive care management and promoting better health outcomes.
- Longitudinal: The “longitudinal” aspect is crucial. An LCP is not limited to a single episode of care or a specific setting. It spans the patient’s healthcare journey over time, ensuring continuity of care and seamless transitions across different providers and facilities.
The Critical Need for Longitudinal Care Programs: Addressing Gaps in Care Coordination
The absence of effective longitudinal care programs contributes significantly to gaps in care coordination, particularly during care transitions. Research has consistently highlighted communication breakdowns and information loss during these transitions as major threats to patient safety.
Insufficient information transfer between care settings can lead to a cascade of negative consequences, including:
- Medical Errors: Incomplete or inaccurate information can result in medication errors, duplicated tests, and inappropriate treatments.
- Care Delays: Providers may need to spend valuable time seeking clarification on patient history and care plans, delaying timely interventions.
- Increased Provider Stress: Lack of information and inefficient communication processes can contribute to provider burnout and dissatisfaction.
- Higher Risk of Rehospitalization: Poorly coordinated transitions can lead to adverse events and a greater likelihood of patients being readmitted to the hospital.
- Patient and Family Frustration: Patients and families often feel lost and uninformed during transitions, leading to anxiety and dissatisfaction with the healthcare system.
Studies have shown that information transferred across settings is frequently incomplete, ambiguous, and delayed. Patients and their families often report a lack of involvement in care transition planning and insufficient information to manage their health at home.
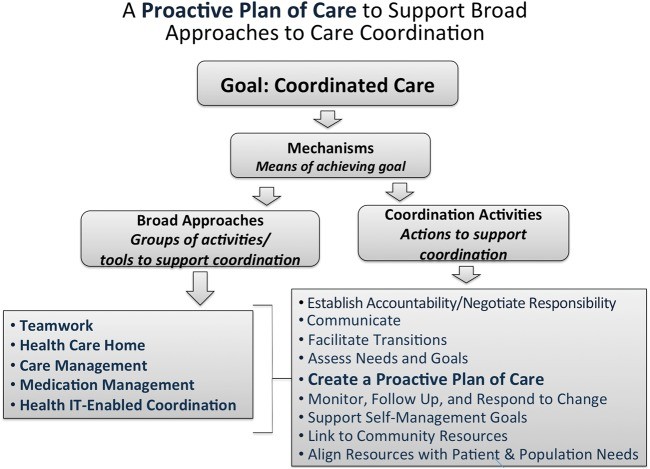
Figure 1: The Agency for Healthcare Research and Quality (AHRQ) Care Coordination Framework, outlining broad approaches and activities for effective care coordination.
Longitudinal care programs, supported by health information technology (HIT), offer a promising solution to bridge these gaps. By ensuring that the right information is available to all stakeholders at the right time, LCPs can significantly improve care coordination and patient safety.
Barriers to Widespread Adoption of Longitudinal Care Programs
Despite the clear benefits, the widespread adoption of longitudinal care programs faces several significant barriers. These challenges span various domains, from definitional ambiguities to practical workflow issues and technological limitations.
Key barriers include:
- Lack of Clarity and Standardization: Confusion surrounding terminology, inconsistent definitions of “care plan” versus “plan of care,” and the absence of standardized content, communication, and messaging standards hinder progress.
- Regulatory and Policy Gaps: While the concept of LCPs is referenced in legislation like the Affordable Care Act and HITECH Act, specific regulatory requirements and incentives for their implementation have been lacking, particularly outside of acute care settings.
- Workflow and Practice Challenges: Integrating LCPs into existing clinical workflows requires significant changes in practice. Developing patient-centered plans, ensuring interdisciplinary collaboration, and establishing processes for sharing, updating, and reconciling plans across settings are complex undertakings.
- Technological Limitations and Interoperability Issues: Current health IT systems often lack the interoperability needed to seamlessly exchange LCP data across different settings and EHR platforms. Many systems are optimized for use within a single setting, hindering the longitudinal aspect of care planning.
- Data Governance and Ownership: Establishing clear guidelines for data governance, patient privacy, and care team member ownership and participation in LCPs is essential but often complex to implement.
- Limited Patient Engagement: Historically, care plans have not consistently been patient-centered. Actively engaging patients and families in problem identification, goal setting, and plan reconciliation is crucial but requires a shift in mindset and practice.
Current State of Longitudinal Care Plan Implementation: Findings from a National Study
To understand the current reality of LCP implementation, a study was conducted across diverse healthcare settings in six regions of the USA. This research involved surveys and interviews with healthcare professionals from emergency departments, acute care hospitals, skilled nursing facilities, and home health agencies. The study aimed to assess the extent to which LCPs are currently used and shared across different levels of care.
Key Findings:
- LCPs are Largely Non-Existent in Practice: Participants across all settings reported that true longitudinal care plans, as defined by a holistic and shared plan across settings, were not in place in their current practice.
- Fragmented Care Plans: While care plans were utilized within individual settings, these were often discipline-specific, setting-specific, and not consistently shared or reconciled across transitions.
- Variability in Care Plan Content and Format: There was significant variation in the types of information included in care plans and the formats used for communication. Even within the same healthcare system, communication often relied on paper and fax.
- Limited Electronic Exchange: Electronic exchange of care plan data, particularly outside of acute care settings, was minimal. When electronic data was exchanged, it was often in unstructured free-text formats, hindering interoperability and data reuse.
- Focus on Meaningful Use Requirements, but Gaps Remain: While some data elements aligned with Meaningful Use requirements (e.g., patient problems, medications, allergies) were more frequently communicated, critical LCP components like patient goals, preferences, and self-management plans were often missing.
Figure 2: Characteristics of healthcare sites participating in the study, highlighting the diversity of settings included in the assessment of LCP implementation.
These findings underscore that the use of LCPs to support care transitions is currently suboptimal, even in technologically advanced healthcare organizations. The “vision” of the LCP as a seamless, shared, and dynamic tool remains largely unrealized.
Moving Towards Effective Longitudinal Care Programs: Strategies for Transformation
Transforming the LCP from an aspirational concept to a practical reality requires a multi-faceted approach, addressing the barriers identified and fostering a culture of collaborative, patient-centered care.
Key strategies include:
-
Standardization and Interoperability:
- Adopting Standardized Definitions: Promoting consistent definitions of “care plan,” “plan of care,” and related terms, such as those proposed by the Standards and Interoperability (S&I) Framework, is crucial.
- Developing Data Standards and Value Sets: Establishing standardized data elements and value sets for LCP components will facilitate electronic exchange and interoperability across systems.
- Leveraging Health Information Exchange (HIE): Promoting the use of HIE platforms to enable secure and seamless sharing of LCP data between different healthcare providers and settings.
- Implementing Consolidated Continuity of Care Documents (C-CCD): Adopting standards like C-CCD to structure and exchange key LCP information electronically.
-
Workflow Integration and Practice Redesign:
- Developing Interdisciplinary Care Planning Processes: Implementing workflows that ensure active participation of all relevant disciplines (physicians, nurses, social workers, therapists, pharmacists, etc.) in LCP development and updates.
- Prioritizing Patient and Family Engagement: Integrating patient and family preferences, goals, and self-management plans into the LCP, and actively involving them in the planning and reconciliation process.
- Establishing Care Plan Reconciliation Processes: Developing clear procedures for reconciling care plans during transitions between settings, ensuring continuity of care and avoiding conflicting plans.
- Training and Education: Providing comprehensive training to healthcare professionals on the principles of LCPs, patient-centered care planning, and the use of relevant technologies.
-
Policy and Incentives:
- Expanding Meaningful Use Incentives: Extending incentives for electronic data exchange and LCP implementation beyond acute care and ambulatory settings to include post-acute care and other relevant providers.
- Developing Quality Measures: Creating quality metrics that incentivize the use of LCPs and reward organizations for achieving improved care coordination and patient outcomes.
- Policy Support for Interoperability: Enacting policies that promote and mandate interoperability of EHR systems and data exchange to facilitate LCP implementation.
-
Technological Advancement and Innovation:
- Developing User-Friendly LCP Tools: Creating intuitive and integrated IT tools that support the creation, updating, sharing, and reconciliation of LCPs within clinical workflows.
- Leveraging Patient Portals and Mobile Health: Utilizing patient portals and mobile health technologies to empower patients to access, contribute to, and manage their LCPs.
- Exploring Innovative Solutions: Investigating and implementing innovative approaches like using problem lists as a foundation for LCPs, incorporating patient goals directly into EHR systems, and utilizing visual displays of care plans for patient engagement.
Figure 3: Example of a group interview guide used in the study, illustrating the focus on care plan components and coordination themes.
Conclusion: Realizing the Promise of Longitudinal Care Programs
What is a longitudinal care program? It is more than just a care plan; it is a paradigm shift towards a truly patient-centered and coordinated healthcare system. Longitudinal care programs hold immense promise for improving patient safety, enhancing care coordination, reducing healthcare costs, and ultimately achieving better health outcomes. However, the current reality is far from this ideal.
This analysis, grounded in research findings, reveals that LCPs are largely a vision rather than a widespread practice. Significant hurdles related to standardization, interoperability, workflows, and policy need to be overcome. Transforming the LCP from vision to reality requires a concerted effort from all stakeholders – healthcare providers, policymakers, technology developers, and patients themselves.
By embracing the strategies outlined, and by fostering a collaborative and innovative approach, we can pave the way for the widespread adoption of longitudinal care programs. This transformation will not only address the critical gaps in care coordination but also empower patients to become active partners in their healthcare journey, leading to a more effective, efficient, and patient-centered healthcare system for all. Future research should focus on evaluating the impact of LCP implementation in integrated care delivery networks, incorporating patient and family perspectives, and refining tools and processes to ensure the successful realization of the LCP vision.